Hepatitis C
- In Switzerland, 32,000 people live with hepatitis C; a third know nothing about their own infection, 200 people die every year as a result of hepatitis C
- The hepatitis C virus is transmitted from blood to blood.
- The symptoms are non-specific, so that those affected often do not associate them with hepatitis C infection.
- Hepatitis C can severely impair quality of life, as it can be accompanied by chronic fatigue, concentration problems or depression.
- New antiviral drugs cure a chronic infection within 8 to 12 weeks; these therapies have few side effects.
Worldwide, around 58 million of the whole population are infected with hepatitis C (HCV). Each year, there are 1.5 million newly infected people. In Switzerland around 32,000 people live with a hepatitis C infection. In developed countries more people die of a hepatitis C infection than of HIV/Aids.
Hepatitis C is often underestimated, as the infection usually proceeds without specific symptoms. Most people who carry the virus are not aware of it for a long time. Cirrhosis of the liver can develop over several years or decades. Public awareness is low despite high numbers of infected people. The World Health Organisation WHO has called it the «silent epidemic».
In only 10 to 20 per cent of all infected people, the virus heals spontaneously. In most cases, a chronic infection manifests itself. 5 to 30 per cent develop liver cirrhosis (scarring of the liver). These people have an increased risk of liver cancer. Chronic hepatitis C is the predominant reason for liver transplants.
Transmission
The virus is transmitted through contaminated blood, especially when materials are exchanged during intravenous or nasal drug use such as syringes, needles, tubes and the like, during tattoos, piercings, manicures or pedicures that are not carried out under sterile conditions, during commercial shaving with insufficiently sterile blades, during blood transfusions or surgical procedures in countries with low hygiene standards and from mother to newborn. Infection via sexual intercourse is rare, except in HIV-positive men who have unprotected sex with other men.
People Most at Risk
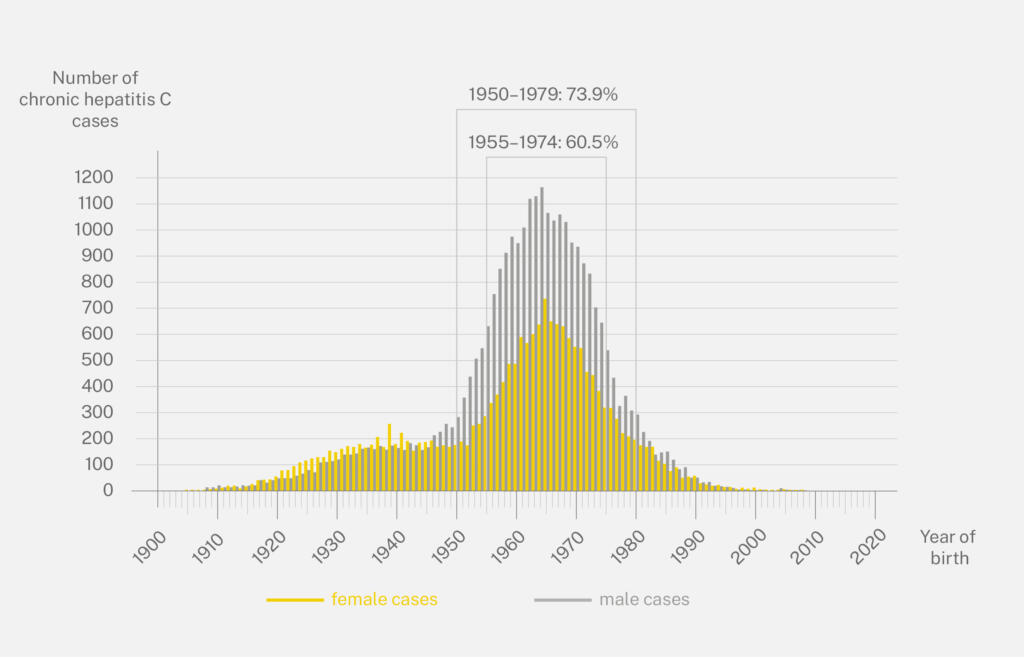
A good half of the infected persons have become infected via drug use. There are also many people who were infected with blood transfusions or during (dental) medical interventions before the virus was discovered. People born between 1950 and 1985 are affected by hepatitis C with above-average frequency.
Symptoms
The incubation period for hepatitis C is two weeks to six months. However, 80 percent of those infected show no symptoms at all in the acute stage. However, acute hepatitis C can be accompanied by fever, fatigue, lack of appetite, nausea, vomiting, abdominal pain, dark urine, grey stools, joint aches and jaundice (yellowing of skin and eyes). If no healing occurs within six months after infection, the acute infection turns into a chronic infection.
The most common symptom of chronic hepatitis C is fatigue. This can be so severe that it severely hampers everyday professional and private life. Other common symptoms are joint pain, pain in the right, upper half of the abdomen, as well as difficulties in concentration and limited performance. The symptoms often appear insidiously, so that many affected persons do not associate them with their hepatitis C infection and only make the connection after successful therapy once the symptoms have disappeared.
Due to the lack of specific symptoms, only a part of the affected people know about the infection. Approximately one third of the 32,000 infected persons in Switzerland are estimated to have no diagnosis.
After hepatitis C is cured, there is no immunity. The person can get infected again.
Diagnosis
Diagnosis is based on the proof of specific antibodies, which the immune system produces against the virus. If there are antibodies in the blood, this means that the body has had contact with the virus. The blood is therefore further tested for the presence of viruses (viral load). Only when viruses are detected is the presence of an active hepatitis C infection confirmed. Hepatitis C antibodies are present for life after contact with the virus, i.e. even after the disease has healed.
In addition, the genetic background of the virus can be determined by applying a complex and expensive method. Today, seven different forms, called genotypes 1 to 7, and over 80 subtypes have been identified. In Switzerland, genotypes 1 to 4 are relevant, genotype 1 being the most common. Since the latest drugs are effective against all genotypes, in most cases a determination is no longer necessary. A total of around 900 to 1000 newly diagnosed chronic hepatitis C cases are reported to the FOPH each year. The number of cases of acute hepatitis C have been stagnating since 1992 at 50 to 65 cases per year. The actual number of new infections is expected to be much higher.
Prevention
There is no vaccine against hepatitis C. The risk of infection can be reduced by not sharing needles, toothbrushes, razor blades and nail clippers. It is advisable to get tattoos or piercings only from tattoo studios that adhere to the hygiene standards of the FOPH.
Treatment
Today, a chronic hepatitis C infection is in most cases easily curable. Until recently, the standard treatment was a combination of interferon and ribavirin. These therapies are physically and mentally taxing. Today, antiviral agents are available that do not require interferon and are highly effective, are accompanied by only a few side effects, and in over 95 percent of cases bring about a cure in 8 to 12 weeks.
With a timely and successful therapy of chronic hepatitis C disease, the liver can largely recover, life expectancy increases and the risk of secondary diseases such as diabetes, kidney damage, stroke or malignant lymph gland cancer decreases. Many people treated today report a noticeable improvement in quality of life due to the disappearance of the unspecific, but stressful symptoms.
Links
- Counselling for people with hepatitis C
Swiss Hepatitis C Association - Leaflet "What is hepatitis C?"
The illustrated leaflet, written in easy-to-understand language, is available in 12 languages and can be ordered from the Swiss AIDS Federation shop.
Studies and articles
-
Birth year distribution in reported hepatitis C cases in Switzerland
Bruggmann P, Richard J-R, on behalf of the Swiss Hepatitis C Cohort Study Group
European Journal of Public Health, Volume 25, Issue 1, February 2015,; 07.11.2015 -
Global epidemiology and genotype distribution of the hepatitisC virus infection
Gower E, Estes C, Blach S, Razavi-Shearer K, Razavi H
Journal of Hepatology2014vol. 61jS45–S57; 30.07.2014 -
Hepatitis C Virus Infections in the Swiss HIVCohort Study: A Rapidly Evolving Epidemic
Wandeler G et al.
Clinical Infectious Disease 2012:55; 15.11.2012 -
Hepatitis C in der Schweiz, epidemiologische Situation 2015–2018
Bundesamt für Gesundheit BAG
BAG-Bulletin 45/2019; 04.11.2019